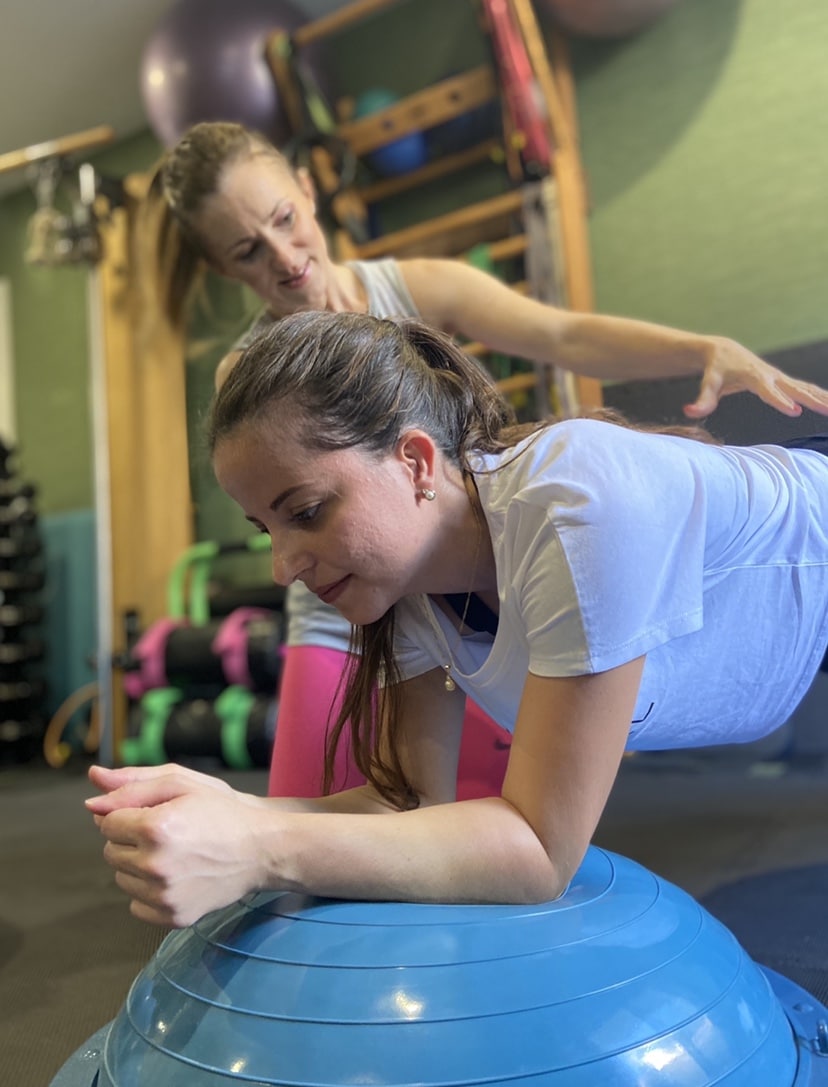
What is proprioception?
Enhancing Body Awareness and Injury Prevention through Proprioception Training Proprioception, often referred to as body awareness, plays a crucial role in our ability to sense

Calcium is a mineral most often associated with healthy bones and teeth, although it also plays an important role in blood clotting, helping muscles to contract, and regulating normal heart rhythms and nerve functions. About 99% of the body’s calcium is stored in bones, and the remaining 1% is found in blood, muscle, and other tissues.
In order to perform these vital daily functions, the body works to keep a steady amount of calcium in the blood and tissues. If calcium levels drop too low in the blood, parathyroid hormone (PTH) will signal the bones to release calcium into the bloodstream. This hormone may also activate vitamin D to improve the absorption of calcium in the intestines. At the same time, PTH signals the kidneys to release less calcium in the urine. When the body has enough calcium, a different hormone called calcitonin works to do the opposite: it lowers calcium levels in the blood by stopping the release of calcium from bones and signalling the kidneys to rid more of it in the urine.
The body gets the calcium it needs in two ways. One is by eating foods or supplements that contain calcium, and the other is by drawing from calcium in the body. If one does not eat enough calcium-containing foods, the body will remove calcium from bones. Ideally, the calcium that is “borrowed” from the bones will be replaced at a later point. But this doesn’t always happen, and can’t always be accomplished just by eating more calcium.
Recommended Amounts
The Recommended Dietary Allowance (RDA) for calcium for women 19-50 years of age is 1,000 mg daily; for women 51+, 1,200 mg. For pregnant and lactating women, the RDA is 1,000 mg. For men 19-70 years of age, the RDA is 1,000 mg; for men 71+ years, 1,200 mg.
Calcium and Health
The reviews below specifically looked at the effect of calcium on various health conditions. Scroll down for links to more information on the health effect of specific foods rich in calcium.
Blood pressure
Cardiovascular disease
Bone health
Colorectal cancer
Kidney stones
Food Sources
Calcium is widely available* in many foods, not just milk and other dairy foods. Fruits, leafy greens, beans, nuts, and some starchy vegetables are good sources.
*Bioavailability of calcium
Calcium is a large mineral and not so easy to break down in the gut. The amount of calcium listed on the Nutrition Facts label of a food product is the measure of calcium in the food, but not necessarily the amount the body will absorb. The amount that is actually absorbed and used by the body is called “calcium bioavailability.” Some foods have higher calcium bioavailability than others.
For example, dairy foods have a bioavailability of about 30% absorption so if a food label on milk lists 300 mg of calcium per cup, about 100 mg will be absorbed and used by the body. Plant foods like leafy greens contain less calcium overall but have a higher bioavailability than dairy. For example, bok choy contains about 160 mg of calcium per 1 cup cooked but has a higher bioavailability of 50%, so about 80 mg is absorbed. Therefore, eating 1 cup of cooked bok choy has almost as much bioavailable calcium as 1 cup of milk. Calcium-fortified orange juice and calcium-set tofu have a similar total amount of calcium and bioavailability as milk, while almonds have slightly lower total calcium and bioavailability of about 20%. This may be useful information for those who cannot eat dairy foods or who follow a vegan diet.
A downside to some plant foods is that they contain naturally occurring plant substances, sometimes referred to as anti-nutrients.” Examples of anti-nutrients are oxalates and phytates that bind to calcium and decrease its bioavailability. Spinach contains the most calcium of all the leafy greens at 260 mg of calcium per 1 cup cooked, but it is also high in oxalates, lowering the bioavailability so that only 5% or about 13 mg of calcium can be used by the body. The takeaway message is not to avoid spinach, which contains other valuable nutrients, but not to rely on spinach as a significant source of calcium since most of it will not be absorbed by the body. You can also schedule your meals so that you do not eat “calcium-binding” foods like spinach at the same meal as calcium-rich foods or with calcium supplements.
If you are scanning food labels to reach a specific amount of daily calcium, continue to aim for the RDAs set for your age group and gender. The RDAs are established with an understanding of calcium bioavailability in food. Also keep in mind that the exact amount of calcium absorbed in the body will vary among individuals based on their metabolism and what other foods are eaten at the same meal. In general, eating a variety of calcium-rich foods can help to offset any small losses.
Signs of Deficiency and Toxicity
Deficiency
Blood levels of calcium are tightly regulated. Bones will release calcium into the blood if the diet does not provide enough, and no symptoms usually occur. A more serious deficiency of calcium, called hypocalcaemia, results from diseases such as kidney failure, surgeries of the digestive tract like gastric bypass, or medications like diuretics that interfere with absorption.
Symptoms of hypocalcaemia:
A gradual, progressive calcium deficiency can occur in people who do not get enough dietary calcium in the long-term or who lose the ability to absorb calcium. The first early stage of bone loss is called osteopenia and, if untreated, osteoporosis follows. Examples of people at risk include:
Guidelines if you are taking calcium supplements for osteoporosis
Toxicity
Too much calcium in the blood is called hypercalcemia. The Upper Limit (UL) for calcium is 2,500 mg daily from food and supplements. People over the age of 50 should not take more than 2,000 mg daily, especially from supplements, as this can increase risk of some conditions like kidney stones, prostate cancer, and constipation. Some research has shown that in certain people, calcium can accumulate in blood vessels with long-term high doses and cause heart problems. Calcium is also a large mineral that can block the absorption of other minerals like iron and zinc.
Symptoms of hypercalcemia:
Did You Know?
Certain nutrients and medications may increase your need for calcium because they either lower the absorption of calcium in the gut or cause more calcium to be excreted in the urine. These include: corticosteroids (example: prednisone), excess sodium in the diet, phosphoric acid such as found in dark cola sodas, excess alcohol, and oxalates.
Source: https://www.hsph.harvard.edu/nutritionsource/calcium/?fbclid=IwAR2C8KrbIqqsPr8mafJX1J5hT9wjp8rqZfrrgb7k2MJOd7Ms-McYTdONFA4
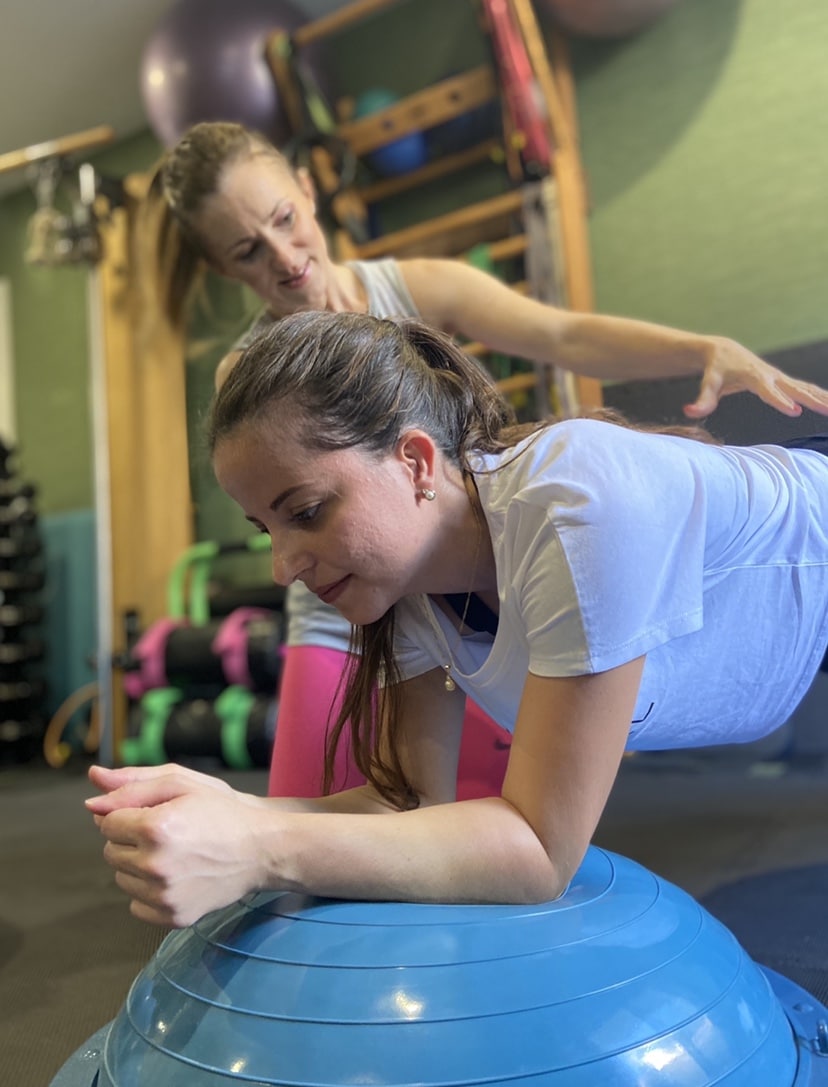
Enhancing Body Awareness and Injury Prevention through Proprioception Training Proprioception, often referred to as body awareness, plays a crucial role in our ability to sense

Hi, I am Andi and I am holistic rehabilitation and movement coach/trainer. I help clients to achieve a healthy, fit body and pain-free lifestyle. Rehabilitation

The vagus nerve is one of 12 cranial nerves in the body. It’s responsible for various bodily functions, including digestion, heart rate, and breathing. Some

The menopause transition is a slippery slope for muscle loss. Here are some key reasons to lift weights to make and maintain as much muscle

Walking with weights can involve either wearable weights or hand weights such as dumbbells. Learn about the different types of weights you can add to

Dear clients ask almost every day how they “need” to sleep. Is there any golden rule for this too!? But there isn’t. Everyone has to